Spider Veins
What Are Spider Veins?
Spider veins can have a weblike appearance or resemble spider legs branching outward, hence the name. In medical terms, they’re called telangiectasias, and they commonly stem from a condition called venous insufficiency. They’re often found on the lower body, presenting as red, purple, or blue clusters of veins.
What Causes Spider Veins?
The most frequent culprit behind spider veins is improper circulation in deeper leg veins which causes spider veins to appear at the surface. Leg veins are tasked with carrying blood back up to the heart once it delivers oxygen to the cells. The veins located deeper within the legs transport the majority of blood, but the superficial, or saphenous, veins near the skin’s surface share some of the work in that upward transit. Leg veins rely on valves that close to keep blood flowing upward and against the gravitational pull downward.
When circumstances cause a valve to fail, the blood leaks backwards, causing pressure, bulging, and the development of new spider veins at the surface. This common occurrence affects nearly half of all men, and over half of all women in the United States. Some patients have no symptoms with spider veins, while others have marked discomfort. Common symptoms include leg heaviness, restlessness, cramps, fatigue, pain, and swelling, which often worsen with prolonged standing or sitting. Exercise and proper posture assist in optimizing circulation and eliminating spider vein symptoms.
Who Is At Risk For Spider Veins?
While spider veins can occur at any age, their onset is primarily in adulthood. Advanced age increases the prevalence. In addition, pregnancy, birth control pills, hormone therapy, leg injury, elevated estrogen levels, obesity, blood clots, and prolonged standing or sitting on the job are risk factors for spider veins. However, the greatest predictor of spider veins is your family history. Individuals whose parents both had spider veins have a 90% likelihood of developing them as well.
What Are the Symptoms of Spider Veins?
Most spider veins are asymptomatic, with the primary complaint being their appearance. But the venous insufficiency that produces spider veins can cause a range of mild to significant symptoms like heaviness, throbbing, cramping, tingling, itching, or burning in your legs. For patients with severe venous insufficiency, symptoms might include ulcerations that heal slowly or discoloration of the skin.
How Do Doctors Treat Spider Veins?
Some spider veins don’t need treatment if they aren’t causing any symptoms. But for symptomatic spider veins, or veins you’d like removed for aesthetic purposes, our vein doctors have excellent solutions, including minimally invasive sclerotherapy.
What Is the Best Treatment for Spider Veins?
Prior to treating spider veins, your vein doctor should evaluate you for venous insufficiency. While spider vein treatment is safe and effective at the surface, untreated vein disease will lead to their recurrence. It’s important to choose a board-certified vein expert to eliminate spider veins completely.
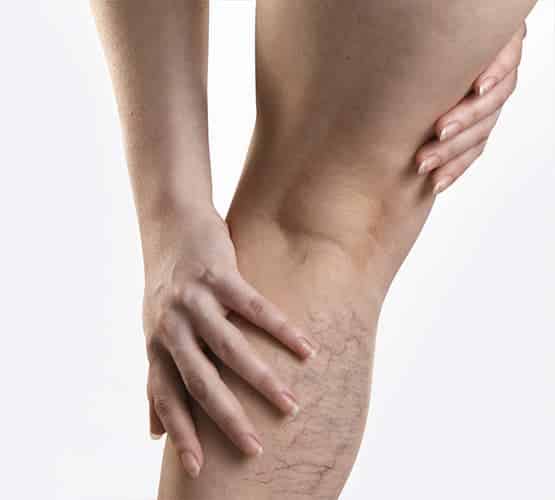
Endоvеnоuѕ Lаѕеr
A safer alternative to vein surgery, this procedure is used to address chronic venous insufficiency. Benefits include an outpatient format with localized anesthesia that eliminates the downtime of surgery.

Radiofrequency Ablation
This minimally invasive form of endovenous ablation uses thermal energy to treat damaged veins. The process is similar to laser ablation, but the heat energy causes less discomfort and bruising than procedures that use laser energy.
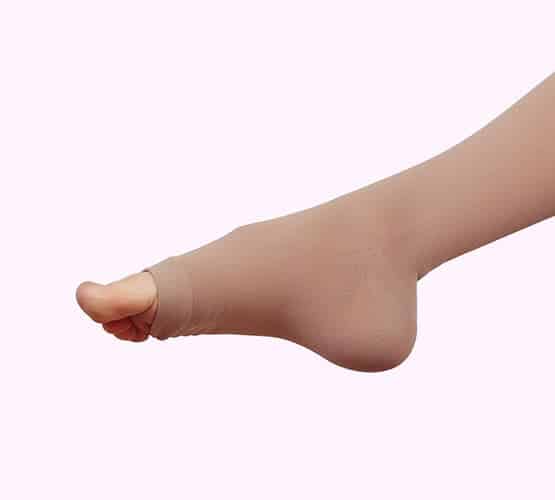
Compression Stockings
Wearing support stockings, or compression stockings, is an easy way to address spider veins at home. The compression enhances blood flow, preventing blood from pooling in the veins. While they won’t change the appearance of spider veins, they will improve the bothersome symptoms and help prevent the development of new spider veins. Proper fitting is essential to ensure safety and efficacy. Have your doctor conduct a formal measurement before buying compression stockings.
Laser Therapy
Diminishing the appearance of spider veins is the primary goal of laser therapy. Our doctors can use laser therapy separately or in conjunction with sclerotherapy as needed for optimal results. This treatment won’t address underlying venous insufficiency and is not recommended for some skin types, so seek laser therapy from a trained physician.
Sclerotherapy
The most common method of eradicating spider veins, this simple procedure is performed in your doctor’s office. Your physician injects an irritant into individual veins to seal the vein’s walls closed, eliminating each damaged vein.

Daily Exercise
Exercise contracts our leg muscles which facilitates blood flow back to our heart. Daily exercise is key to maintaining adequate circulation. While exercise won’t eliminate existing spider veins, it will prevent new ones from forming. In addition, those with venous insufficiency should avoid sitting or standing for long periods of time. Talk to your doctor about simple tips like elevating your legs while seated or lying down to reduce pressure and swelling in the veins.